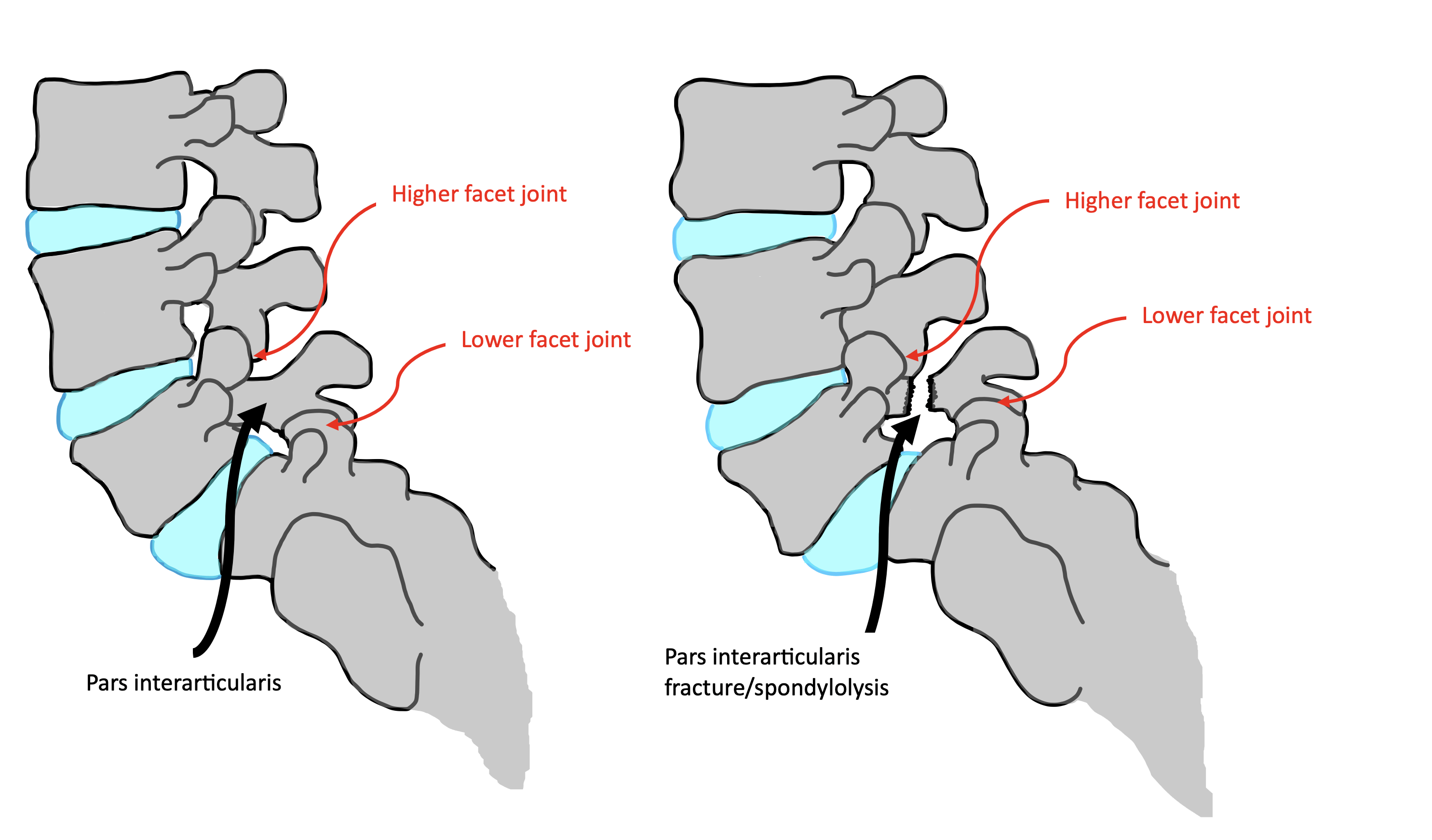
When people think about spinal pain or stiffness, attention often goes straight to the neck or lower back. But sitting right in the middle is an area that plays a huge role in how we move, breathe, and perform every day – the thoracic spine!
The thoracic spine refers to the mid-back region, made up of 12 vertebrae connected to the ribs. This area is designed for both stability and movement. It helps support posture, allows rotation and extension through the trunk, and protects vital organs including the heart and lungs.
Why Does the Thoracic Spine Become Stiff?
Modern lifestyles don’t do the thoracic spine many favours. Long hours sitting at desks, driving, studying, doomscrolling and repetitive sport positions can all encourage us into rounded postures over time.
When the thoracic spine spends prolonged periods in flexed or slouched positions, the surrounding joints, muscles, and connective tissues can gradually lose mobility. Many people begin to notice:
> Mid-back stiffness or tightness
> Neck tension or headaches
> Shoulder discomfort
> Difficulty rotating during sport
> Feeling “stuck” when trying tog to stand upright
Athletes can also develop thoracic stiffness from repetitive loading patterns. Cyclists, swimmers, runners, desk workers, and gym-goers commonly develop reduced mobility through the region due to the positions they spend the most time in.

Why Thoracic Mobility Is So Important
The thoracic spine is designed to rotate, extend, and move with breathing. When mobility is reduced, other areas of the body often compensate.
For example:
> Limited thoracic extension can increase load on the neck and shoulders
> Poor rotation can place extra stress through the lower back
> Restricted rib movement can affect breathing efficiency
> Shoulder movement can become limited if the upper back cannot move properly
Good thoracic mobility helps the body distribute load more efficiently. This becomes especially important running, throwing sport, swimming, lifting, golf, tennis, and even everyday tasks like reaching overhead or turning when driving.
The Link Between the Thoracic Spine and Breathing
One of the most overlooked roles of the thoracic spine is its relationship with breathing.
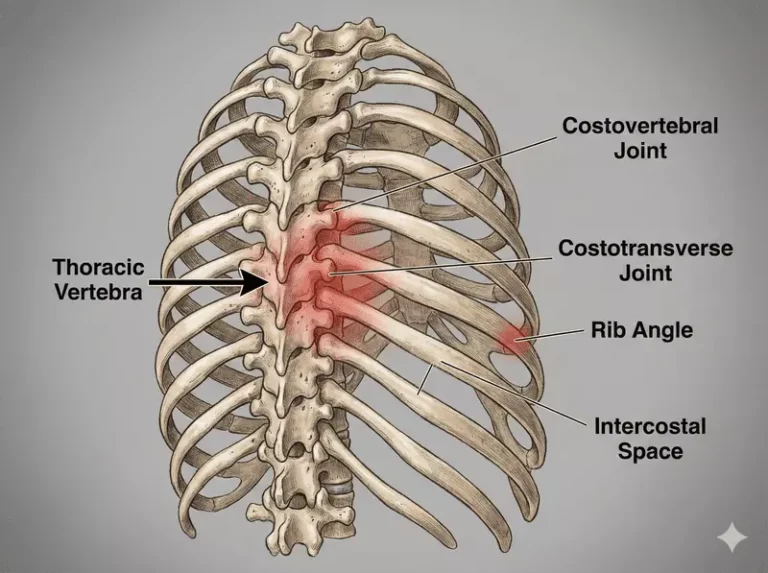
The ribs attach directly to the thoracic spine, meaning every breath requires movement through this area. During the efficient breath, the rib cage should expand in multiple directions while the diaphragm works alongside the the abdominal muscles and pelvic floor to manage pressure within the trunk.
When the thoracic spine and rib cage become stiff, breathing mechanics can change. People may begin to rely more heavily on shallow chest breathing, overuse the neck and upper shoulder muscles, or struggle to take full deep breaths during exercise.
Poor breathing can contribute to:
> Increased neck and shoulder tension
> Reduced exercise efficiency
> Feelings of stiffness through the chest and upper back
> Difficulty relaxing the nervous system
> Poor trunk pressure management during lifting or management
More Than Just Movement: Protection and Support
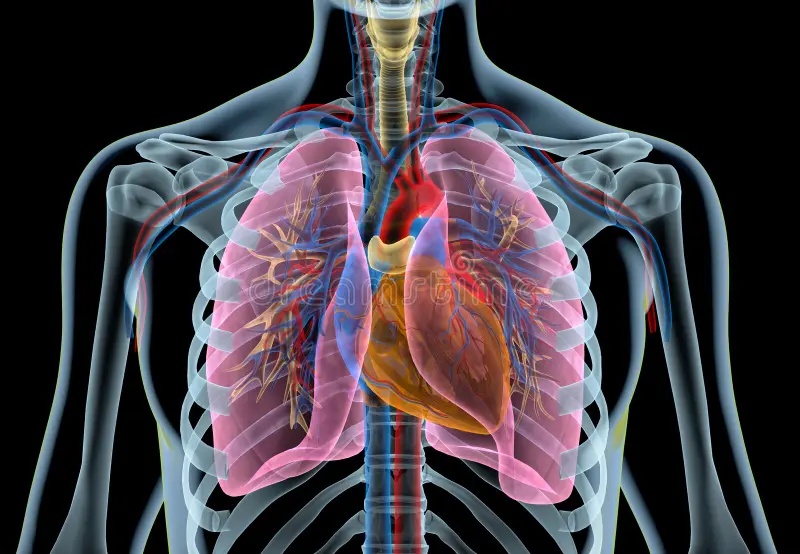
The thoracic spine also has an important protective role. Together with the rib cage, it forms a strong structure around vital organs including the heart and lungs.
Because of this protective role, the thoracic spine is naturally a little stiffer than the neck or lower back. It’s designed to provide stability while still allowing enough movement for breathing and rotation.
The goal isn’t excessive flexibility – it’s balance mobility, strength, and control
How Can You Keep Your Thoracic Spine Healthy?
Some simple ways to support thoracic mobility and function include:
> Regular movement breaks from sitting
> Rotational and extension-based mobility exercises
> Strengthening the upper back and trunk muscles
> Improving breathing mechanics
> Gradually progressing training loads
> Maintaining variety in movement throughout the day
If you’re experiencing persistent mid-back stiffness, neck tension, restricted movement, or discomfort during sport or exercise, assessment from a physiotherapist can help identify what may be contributing and guide an appropriate management plan.
Your thoracic spine does far more than just “sit in the middle” of the body – it plays a key role in movement, breathing, posture, performance, and overall function every single day.